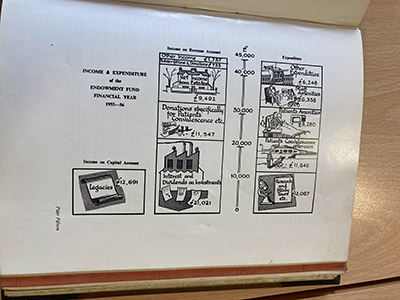
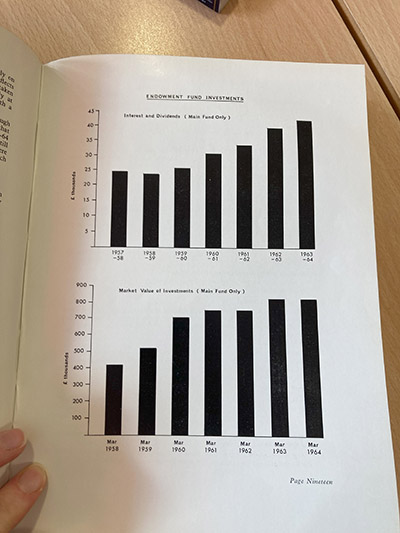
In Part 6 of the Hospital Charity takeover, Nora Kenworthy shares two poems from her recently published book Crowded Out (2024), where health care crowdfunding campaign narratives become evocative choruses.

For nearly a decade, I have studied the use of crowdfunding sites like GoFundMe to raise money for health care needs in the US. My work in this domain marries intimate ethnographic inquiry with large, data-driven analyses to document the broad contours of inequity in the crowdfunding ecosystem. Doing this work requires reading and engaging with thousands of GoFundMe narratives on different topics. In addition to exploring individual stories of crowdfunding experiences, I wanted to find a way to convey to broader readers the unique form and affect of crowdfunding appeals, which are both highly personal and very public. While these narratives frequently follow similar styles and conventions, and express similar affective experiences, they also share intimate details of crowdfunder and patient lives, stories, struggles, and identities.
I began writing composite, found poetry from snippets of text on different GoFundMe campaign pages as a way to make sense of, and convey, these unique narrative characteristics. I wanted to capture the remarkable alignments and frictions that arise among narratives, which are so often encountered individually, but to the researcher begin to sound like a haunting chorus of repeated phrases, appeals, and needs. I also wanted to find ways to capture the unique elements of many of these narratives while offering users a greater measure of privacy than they were able to find through online crowdfunding.
The lines and stanzas of these poems are made up of text from many different crowdfunding narratives collected throughout my research. Text fragments are compiled into the poem through paraphrasing or splicing such that they cannot be traced back to their original campaigns. I used reverse online searches of each text fragment to ensure confidentiality.
The two poems below explore common discursive and affective elements of crowdfunding narratives in the US milieu: (1) appeals to personal goodness and (2) having to set aside one’s pride. These themes relate to a central point of inquiry in my work on crowdfunding’s “moral toxicities” and how these relate to broader social mores about asking for help and receiving it in late liberal systems. The poems use repetition of similar but unique phrases to evoke a choral effect. This repetition creates a collective experience intended to counteract crowdfunding’s highly individualized and marketized experiences for users. At the same time, differences in pitch, tone, and syntax remind the reader (I hope) of these uniquely human stories.
[1] Very good people
First of all, we ask for your prayers for Emily’s healing.
Emily is a very good person who loves the Lord and her family.
This is the story of a spectacular human,
one of the most tenderhearted, understanding,
funny, loving, upbeat,
loyal, ambitious, optimistic,
charismatic, tenacious,
one of the kindest, friendliest, biggest-hearted,
people on the planet.
The best human being
I’ve ever known.
A hard worker and good person
who loves his family very much.
A good person with a big heart
who just wants to survive to help others.
Who works two jobs
and takes care of her grandkids.
Who works his hands to the
bone everyday to feed three daughters.
Who never quits, even when
there are many cases of COVID at work.
Who was pulling himself up by the bootstraps
when Big C cut the straps.
We were promised the American dream,
that bad things don’t happen
if you work hard, do well,
are a good person.
It doesn’t matter to cancer that you’ve been a good person.
That you’re a father, a mother, someone’s child
a caring daughter, supportive sister, devoted partner
a loving dog mom
a champion of underdogs
a gifted teacher
an army medic
a widower
a hardworking tree lover
a phlebotomist police officer
a talented and kind lawyer
or that you’re only 30 and a very good person,
but can’t afford the transplant.
Cancer doesn’t care.
It doesn’t matter if you’re rich or poor,
educated or not,
that you’re 31 years old
and the sole breadwinner for your family.
This process
of proving your worth
and your right to claim it
is humiliating
and only sometimes fruitful.
[2] A matter of pride
Hello.
Yeah, I’m still here.
I pray I’ll find the right words to tell this story.
I’d never do this but I’m swallowing my pride
This might be the hardest thing I’ve ever had to write.
But here we are (swallowing pride)
Okay let’s try this again. I cancelled the last one
within minutes because . . .
well, to put it simply, pride.
I’m simply trying to survive, pushing past my pride
I have no idea how to do this
without completely debasing myself.
The only thing bigger than his heart is his pride
So many people have asked
how they can help and I
keep saying, “we’re fine, we’re fine.”
But we are not fine.
I am putting our pride on the back burner
That fact I even have to start
a GoFundMe is hitting my pride lol, but
I was told to reach out if I needed help.
Friends, now I need it.
Here I am, with humility and swallowed pride
Desperation makes us do
things we might not do otherwise, but
desperation is now my reality.
It was bad enough to beg for money
the first time, and I’m even more ashamed now.
I’ve conceded trying to swallow my pride
No one likes to admit publicly they are struggling,
have lost or failed or are in pain.
That we need help.
But I’m coming to you with my pride set aside
It pains me to ask this—
pains, and shames me.
I’m tossing my stubborn pride out the window
For the first time in this battle I am really scared.
My savings are gone and I’ve no more income.
I’ve learned the hard way to swallow my pride
Gradually, we’ve redirected every single
penny to medical expenses
I shouldn’t let pride keep me from asking for help . . . right??
Her life is on the line if we can’t pay for this surgery.
Our pride’s gotta jump out the window
This is how hardworking people end up on the street.
Not sure whether I should be shamed or optimistic
this is not the American dream,
it’s my American nightmare
It feels greedy to ask for what I need
But I know of no other way.
Maybe we’re all in this together, maybe
hardship teaches us to rely on one another.
Anyways, I have cancer. Again.
Postscript
The above passages are excerpted from Crowded Out: The True Costs of Crowdfunding Healthcare by Nora Kenworthy. Reprinted with permission from The MIT Press. Copyright © 2024.
About the author
Nora Kenworthy is a Professor of Nursing and Health Studies at the University of Washington Bothell. Her work—including her recently published book Crowded Out (2024)—examines how politics, technology, and inequality affect health.